Healthcare sounds simple in theory.
You get sick. You see a doctor. You get treated.
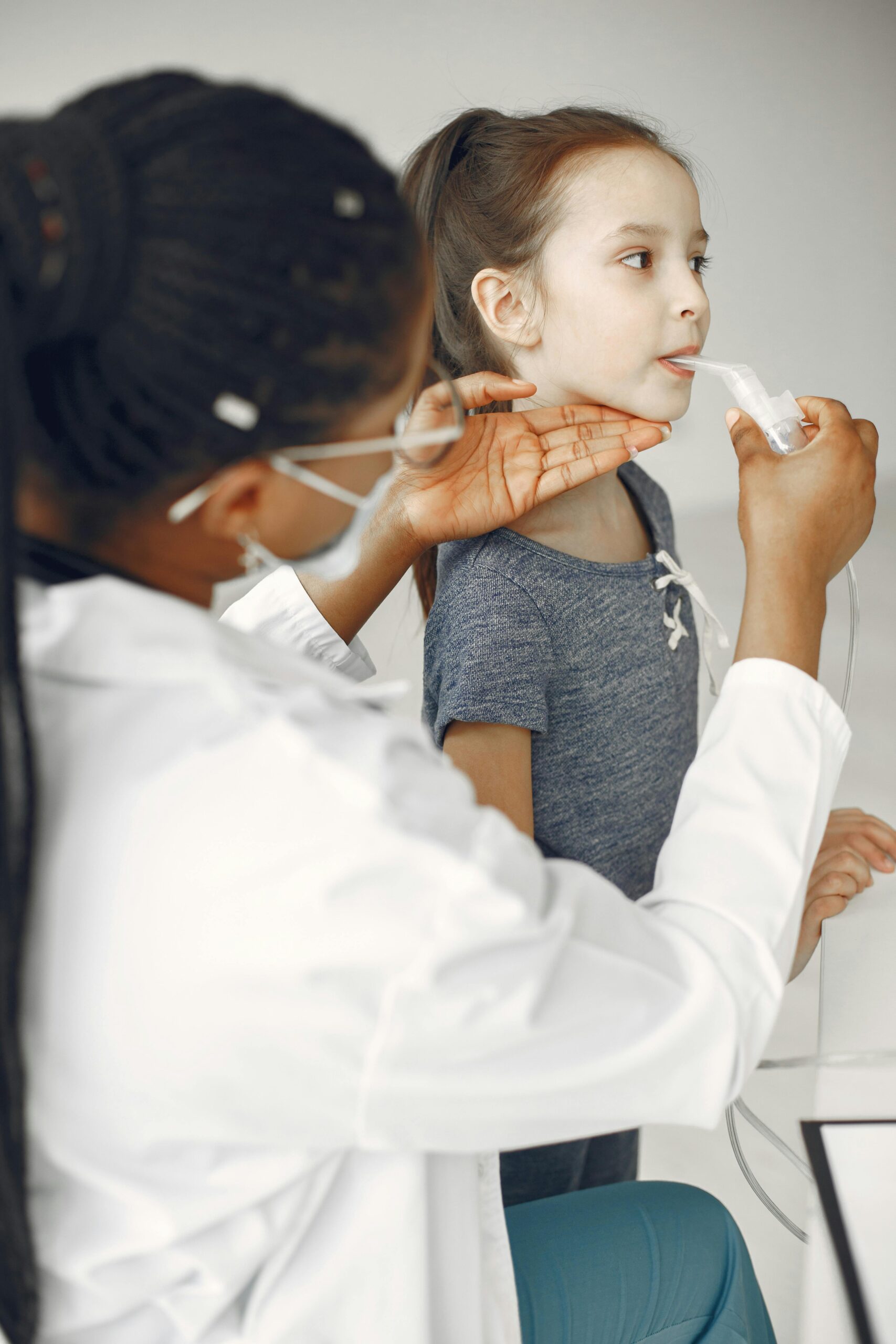
But real health does not work that way. Health unfolds over months and years. It shifts with stress, age, work pressure, travel, family history, and environment. In fast-growing African cities like Lagos, Nairobi, and Johannesburg, lifestyle diseases are rising.
Hypertension, diabetes, burnout, and heart disease are no longer rare. This is where continuous care becomes powerful. It is relationship-based healthcare.
In our main guide on 7 Powerful Reasons Continuous, Relationship-Based Care Is the Future of Healthcare, we explained why this model matters. In this article, we answer a more practical question: What does continuous care actually look like in real life?
Not theory.
Not buzzwords.
Real practice.
Continuous Care Is Not “More Visits.” It Is Smarter Oversight.
Many people assume continuous care means going to the doctor every week. It does not. It is about consistency, not frequency. Continuous care means:
- one named physician
- long-term relationship
- clear follow-up structure
- ongoing oversight
- coordinated decision-making
1. Named Doctor Who Knows Your Baseline
In fragmented systems, patients repeat their story at every visit. In continuous care:
- the doctor knows your history
- your medications are familiar
- your past test results are understood
- your lifestyle is remembered
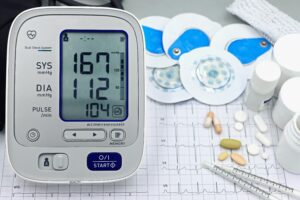
This matters because medicine depends on trends. A blood pressure of 135/85 means different things for a 28-year-old athlete and a 52-year-old executive under stress. When your doctor knows your baseline, small changes become visible early.
2. Structured Follow-Up, Not “Come Back If It Gets Worse”
In transactional care, patients are often told, “Return if symptoms continue.” In relationship-based care, follow-up is planned intentionally. This reduces complications. For example:
- blood pressure review in 4 weeks
- repeat lab review after medication adjustment
- lifestyle reassessment after 3 months
The WHO consistently emphasizes that strong primary care and longitudinal follow-up reduce avoidable hospital admissions globally. Follow-up is not optional. It is protective.
3. Chronic Disease Monitoring Over Time
Africa is seeing rapid growth in non-communicable diseases. According to the WHO, hypertension and diabetes are increasing significantly across sub-Saharan Africa. These conditions cannot be managed safely through isolated visits.
Continuous care in practice is not dramatic. It is steady. And steady saves lives. It includes:
- medication tracking
- lab trend monitoring
- lifestyle coaching
- adjustment of treatment plans over time
4. Preventive Screening That Happens on Time
In fragmented systems, screenings are often missed. In continuous care, your doctor tracks:
- age-appropriate screenings
- family history risks
- vaccination schedules
- cancer screening timelines
These are scheduled proactively, not reactively. Prevention only works when someone is watching the timeline. For example:
- colon cancer screening after age 45–50
- prostate discussions based on family risk
- cardiovascular risk assessment in midlife
5. Context-Based Advice, Not Generic Advice
Online health advice is often broad and impersonal. Continuous care changes that. A senior executive flying weekly across Africa has different health needs than someone working remotely. Context shapes care. Advice becomes tailored to:
- job demands
- stress load
- travel frequency
- sleep pattern
- diet habits
6. Coordination When Specialists Are Needed
Continuous care does not eliminate specialists. It organizes them. When a referral is required:
- primary doctor explains why
- medical records are shared clearly
- results are reviewed together afterward
- long-term plan is adjusted
Relationship-based care reduces these risks. Without coordination, patients can receive:
- conflicting advice
- duplicate prescriptions
- repeated tests
7. Monitoring Between Major Events
Continuous care includes oversight even when you feel fine. This kind of monitoring prevents the silent progression of disease. Hypertension is often symptomless. So is early diabetes. Without oversight, these conditions can quietly advance. Examples:
- reviewing annual labs
- tracking weight changes
- monitoring stress levels
- checking medication tolerance
8. Clear Accountability
In fragmented systems, responsibility is unclear. In continuous care, accountability improves safety. When someone “owns” the big picture, errors decrease.
- one physician remains accountable
- clarity about who to contact
- follow-up does not fall through the gaps
9. A Long-Term Health Strategy
Continuous care is strategic. This approach is especially valuable for high-performing professionals who want to maintain energy, clarity, and productivity long-term. Instead of solving isolated problems, your doctor works with you on:
- 5-year risk planning
- cardiovascular risk reduction
- weight management goals
- stress resilience
- healthy aging
Health becomes an asset to manage, not a crisis to fix.
Continuous Care Does NOT Look Like
To avoid confusion, continuous care is not:
- random online doctor chats
- anonymous call-center medicine
- replacing in-person evaluations when needed
- ignoring specialist expertise
It is about strengthening the relationship with your own physician and improving coordination across your care journey. It is structured. Responsible. Personal.
Day-in-the-Life Example
Let’s make this practical. Imagine a 45-year-old business leader in Nairobi. Under fragmented care:
- He visits urgent care for headaches.
- Sees another doctor for annual labs.
- Gets stress medication from a third clinic.
- No one connects the dots.
Under continuous care:
- His primary doctor tracks his rising blood pressure.
- Notices weight gain over 3 years.
- Screens for sleep issues.
- Adjusts lifestyle plan early.
- Prevents long-term complications.
Same patient. Different outcome.
Continuous Care Model Is Growing Globally
The World Bank has highlighted the economic value of strong primary care infrastructure in improving health system efficiency. Countries with strong primary care systems consistently show:
- lower healthcare costs
- better chronic disease outcomes
- higher patient satisfaction
Continuous care is not only medically smart. It is economically responsible.
Continuous Care Benefits African Urban Professionals
Urban African professionals face long work hours, high stress, traffic and commuting strain, and rising lifestyle disease risk. Continuous care is proactive protection in an otherwise demanding environment. It supports:
- early cardiovascular monitoring
- stress management oversight
- regular metabolic screening
- long-term health planning
ChextrMD and the Rise of Premium Continuous Care
As healthcare shifts toward continuity and long-term partnerships, new care models are emerging to support this evolution responsibly. One example is ChextrMD.
ChextrMD is not telemedicine.
It does not connect patients to random doctors.
It does not replace in-person evaluations.
Instead, it supports something far more valuable: continuous access between physicians and their own known patients.
👨🏻⚕️ Built Around Existing Doctor–Patient Relationships
ChextrMD is designed to strengthen established medical relationships. This preserves what matters most—trust, familiarity, and accountability. It enables:
- ongoing physician oversight
- structured follow-up between visits
- secure communication within an existing care relationship
- better monitoring of trends over time
In fragmented systems, patients often struggle to maintain consistent communication with their primary doctor. ChextrMD supports continuity of care by helping physicians remain accessible to the patients they already know and understand.
🧖♂️ Designed for High-Trust, High-Responsibility Care
The model aligns especially well with these individuals, who often require more than occasional appointments. They benefit from premium follow-up, closer monitoring, and a clear medical partnership. This refers to:
- busy executives
- high-income professionals
- families seeking structured long-term care
- patients managing chronic conditions
ChextrMD strengthens this partnership without disrupting it.
🧑🧒🧒 Supporting Oversight, Not Replacing Clinical Judgment
Importantly, ChextrMD does not encourage self-diagnosis or unsupervised treatment. It reinforces the role of the physician as
- long-term medical advisor
- monitor of evolving health trends
- coordinator of specialist care
- consistent point of accountability
The platform exists to make continuity practical in modern life—especially in fast-moving urban environments across Africa, where time constraints and system strain can otherwise interrupt follow-up.
👜 Technology Serving Relationships, Not Replacing Them
The future of healthcare is not anonymous digital consultations. It is technology that supports real doctor–patient relationships. ChextrMD reflects this shift.
ChextrMD helps physicians maintain structured communication and oversight with their known patients, ensuring that care remains personal, continuous, responsible, and safe.
In a world of fragmented encounters, strengthening existing medical relationships is not only innovative—it is essential.
Continuous, relationship-based care is the future.
ChextrMD is one example of how that future can be supported responsibly.
FAQs: What Continuous Care Looks Like in Practice
Q1: How often do I need to see my doctor in a continuous care model?
There is no fixed schedule for everyone. It depends on your health profile—your age, medical history, lifestyle, and risk factors. Some patients may need quarterly reviews. Others may need structured annual check-ins. For example:
- A healthy 30-year-old may need structured annual reviews.
- A 50-year-old with hypertension may need quarterly monitoring.
- Someone adjusting to a new medication may require short-term follow-up.
The key is not how often you visit. The key is that your visits are planned and connected, not random. Continuous care creates a rhythm of oversight that matches your real needs.
Q2: What happens between visits?
This is where continuous care truly stands out. You are not “forgotten” after the appointment ends. Your care plan continues moving forward, even when you feel well. Between visits, your doctor may:
- review lab results and trends
- adjust recommendations if needed
- monitor ongoing treatment response
- plan the next checkpoint
This reduces the silent progression of conditions like high blood pressure, prediabetes, and high cholesterol. Ongoing oversight prevents surprises.
Q3: Can continuous care work if I travel frequently?
Yes. In fact, it works even better for frequent travelers. Business leaders and professionals who move between cities like Accra, Kigali, or Cape Town often experience these travel-related risks:
- sleep disruption
- stress spikes
- irregular meals
- missed checkups
A long-term doctor understands these patterns and adjusts care accordingly. Instead of starting from zero in every new location, your medical history remains anchored and consistent. Continuity becomes stability in a mobile life.
Q4: Does continuous care replace emergency services?
No. Emergency services remain essential. If you have severe chest pain, sudden weakness, difficulty breathing, or trauma, you must seek urgent care immediately. Continuous care reduces the likelihood of preventable emergencies by:
- monitoring risk factors
- adjusting treatment early
- catching warning signs before they escalate
It complements emergency services. It does not replace them.
Q5: What if I rarely get sick?
That is exactly when continuous care has the most value. Many serious conditions begin quietly. Prevention works best before symptoms appear. Staying healthy requires oversight, not luck. When you rarely get sick, your doctor can:
- establish a strong health baseline
- track subtle changes over time
- keep screenings up-to-date.
- guide preventive lifestyle adjustments
Q6: Is continuous care only for older adults?
No. Building a doctor–patient relationship early in adulthood creates long-term protection. It is easier to maintain health than to rebuild it. While older adults benefit greatly due to higher health risks, younger professionals also gain from:
- early cardiovascular risk assessment
- stress and burnout monitoring
- reproductive health planning
- fitness and nutrition guidance
Q7: What role does prevention really play?
Prevention is central. The WHO consistently highlights prevention and strong primary care as critical pillars of the global success of health systems. Prevention works when someone is consistently watching the timeline. Continuous care supports:
- blood pressure trend monitoring
- blood sugar tracking
- cancer screening planning
- vaccination updates
- lifestyle coaching
Q8: Is this model realistic in African healthcare systems?
Yes, and it may be even more necessary. In many African cities, hospitals are busy, and access to specialists may be limited. Strong primary relationships stabilize fragmented systems. Continuous care provides:
- clear entry into the system
- better referral coordination
- reduced duplication of tests
- earlier management of chronic disease
Q9: What should I look for if I want continuous, relationship-based care?
Continuity should feel organized, safe, and personal. Look for:
- named physician responsible for your long-term care
- clear follow-up plans after visits
- coordination when specialists are involved
- emphasis on prevention and monitoring
- consistency over time
Avoid systems where:
- you never see the same doctor twice
- no one tracks your long-term trends
- advice feels generic or disconnected
Q10: Is continuous care suitable for high-performing professionals?
Yes. In fact, high-performing professionals often benefit the most. Long work hours, high stress, and frequent travel increase health risks over time. For busy leaders, health becomes an asset that must be managed intentionally. Continuous care provides:
- early cardiovascular monitoring
- stress-related health oversight
- strategic long-term planning
- trusted medical partner
Continuous Care Is Active, Not Passive
Continuous care is not about more appointments. It is about a smarter connection over time.
It brings clarity to complex systems.
It builds trust in uncertain moments.
It turns healthcare from reactive to proactive.
And most importantly, it ensures that someone who truly knows you remains accountable for your health journey. Always work closely with your own trusted physician—someone who knows you, understands your history, and walks with you long-term.
Health is not built in single appointments.
It is built on relationships.
This is what continuous care looks like in practice. 👩❤️👩🩺