Hypertension, Diabetes, and Asthma Matter Together
Hypertension, diabetes, and asthma look different on the surface.
One affects blood pressure. One affects blood sugar. One affects breathing.
But they share a dangerous trait. They can worsen quietly. People often feel “fine” right up until a crisis happens. A stroke. A severe asthma attack. A diabetic emergency.
This is why clinical monitoring tied to continuity of care is not optional for these conditions. It is protective.
This guide explains how monitoring works when done correctly, why continuity makes it safer, and how doctors use trends over time to prevent avoidable emergencies.
Hypertension, Diabetes, and Asthma Need Long-Term Monitoring
These conditions:
- change slowly
- fluctuate day to day
- influenced by stress, diet, weather, sleep, and routine
- respond differently in different people
A single clinic reading tells very little. What matters is pattern, not point. Continuity allows a clinician to:
- know the patient’s usual range
- detect early drift
- adjust care before damage occurs
Monitoring without continuity creates data. Monitoring with continuity creates protection.
🩸 Monitoring Hypertension: Catching Danger Before Symptoms Appear
Blood Pressure is Called the “Silent Killer”
High blood pressure rarely causes pain. It damages the brain, heart, kidneys, and eyes. Many patients feel normal while damage accumulates. This makes regular monitoring essential, not optional.
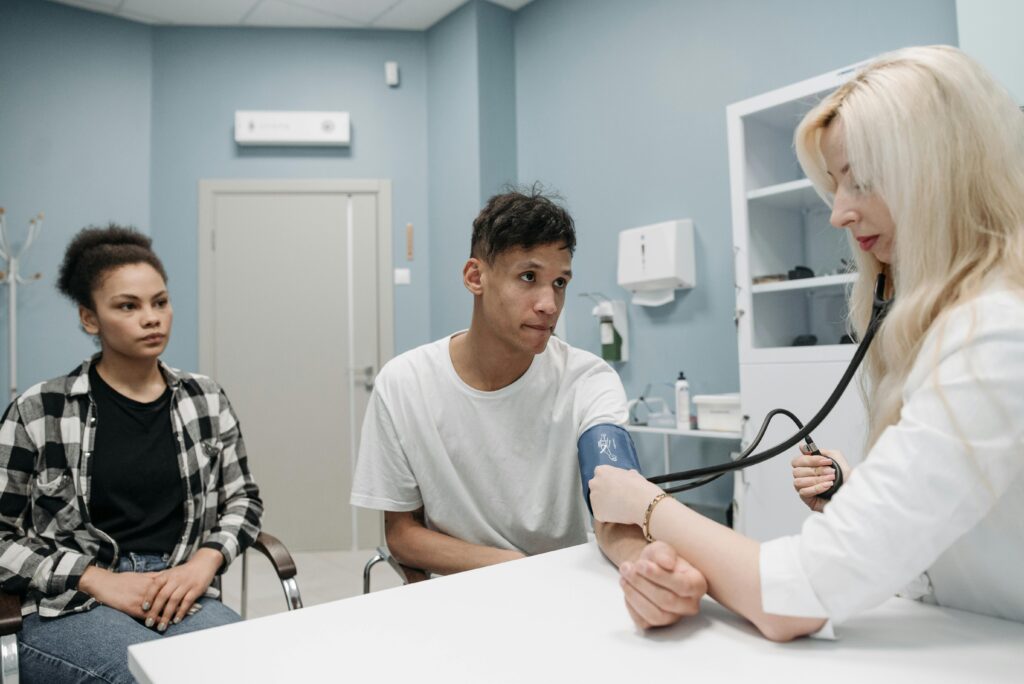
What Effective Blood Pressure Monitoring Looks Like
Good monitoring includes:
- repeated readings, not one-off checks
- home measurements taken correctly
- trend review by the same clinician or care team
A common and safe approach:
- measure BP twice daily for 5–7 days
- repeat monthly or as advised
- bring or send readings to the same doctor
Continuity matters because:
- some patients always run higher in clinics
- others have masked hypertension
- stress patterns differ
A doctor who knows the patient can tell the difference.
Common Monitoring Mistakes in Hypertension
- reacting to a single high reading
- changing medication without trend context
- ignoring low readings in treated patients
- using poorly calibrated home devices
These errors happen more often when care is fragmented.
🩸 Monitoring Diabetes: Trends Matter More Than Numbers
Diabetes Monitoring is More Than Blood Sugar Checks

Diabetes affects the blood vessels, nerves, kidneys, eyes, and heart. Damage builds over time. Monitoring must look at:
- daily glucose patterns
- long-term control (HbA1c)
- symptoms
- medication tolerance
A clinician who follows the patient over the years can see:
- whether control is improving or slipping
- how lifestyle changes actually work for that person
- when medication changes are truly needed
Key Elements of Diabetes Monitoring
Effective diabetes monitoring includes:
- home glucose checks (frequency depends on treatment)
- HbA1c every 3–6 months
- weight and blood pressure tracking
- review of hypoglycemia symptoms
Diabetes is not just about lowering numbers. It is about lowering risk safely. Continuity allows doctors to:
- adjust targets safely
- prevent overtreatment
- reduce low blood sugar episodes
Continuity Prevents Diabetes Complications
When the same clinician monitors diabetes:
- medication changes are cautious and informed
- small warning signs are noticed
- adherence discussions are honest
Trust improves control. Patients are also more likely to:
- report symptoms early
- admit challenges with diet or routine
- stay engaged long term
🩸 Monitoring Asthma: Watching Patterns, Not Just Attacks
Asthma Needs Ongoing Monitoring Even When Symptoms are Mild

Asthma severity can change quietly. Triggers include dust, pollution, cold air, stress, and infections. A patient may feel “okay” while lung function slowly declines. Monitoring helps doctors:
- adjust prevention therapy early
- reduce emergency attacks
- keep airways stable
Asthma Monitoring Should Include
Good asthma monitoring includes:
- symptom frequency tracking
- night-time symptoms
- rescue inhaler use
- peak flow readings (where appropriate)
Asthma control is dynamic. Continuity keeps it that way. Continuity allows clinicians to:
- recognize seasonal patterns
- identify personal triggers
- adjust treatment before flare-ups
Dangers of Fragmented Asthma Care
When asthma care is fragmented:
- controllers are underused
- relievers are overused
- warning signs are missed
One team following the patient reduces this risk. Seeing different clinicians often leads to:
- inconsistent plans
- poor inhaler technique review
- repeated emergencies
Monitoring Works Better When One Team Oversees All Three Conditions
Many patients have more than one chronic condition. Hypertension and diabetes often coexist. Asthma may sit alongside them. Continuity allows doctors to:
- balance medications safely
- avoid drug interactions
- prioritize what matters most
A clinician who knows the full picture can make careful adjustments. For example:
- steroids for asthma can raise blood sugar
- some BP drugs affect glucose control
Monitoring Plans Should be Simple, Not Overwhelming
Over-monitoring causes fatigue. Good plans are:
- easy to follow
- clearly explained
- linked to clear actions
The best plans fit real life. Examples:
- “Check BP twice daily for 7 days every month”
- “Check fasting glucose 3 times a week”
- “Track asthma symptoms daily for 2 weeks during season changes”
Clinicians Interpret Monitoring Data Over Time
Monitoring creates data. Continuity creates understanding. A rising trend over months means something different from one bad week. This longitudinal view protects patients from overreaction and underreaction. Doctors look for:
- direction (up, down, stable)
- variability (wide swings vs steady control)
- context (illness, stress, missed doses)
Clinics Can Improve Outcomes
Small changes compound over time. Clinics can start by:
- assigning named clinicians or teams
- standardizing monitoring plans
- creating simple escalation rules
- tracking outcomes
Role of Nurses and Care Coordinators
Continuity does not mean only the doctor is involved. Safe models include:
- nurses reviewing readings first
- coordinators checking adherence
- doctors focus on decisions
Ownership stays clear. This team-based continuity:
- improves response time
- reduces physician overload
- keeps care personal
Technology Can Help, But Only With Continuity
Devices and apps can:
- collect readings
- send reminders
- flag abnormalities
But they must connect to the patient’s known clinician or a familiar care team. Disconnected dashboards increase noise and anxiety. Technology should support relationships, not replace them.
Special Considerations in African Health Contexts
In many African settings:
- devices may be shared
- clinics may be busy
- follow-up may be irregular
What matters is consistency, not complexity. Continuity can still work through:
- community health workers
- scheduled monitoring days
- SMS check-ins
- simple paper records
Monitoring Hypertension, Diabetes, and Asthma: What Patients Should Know
Patients should understand:
- why is monitoring recommended
- what numbers matter
- when to report changes
- who is responsible for follow-up
Engaged patients have better outcomes. Good questions to ask:
- “Who reviews my readings?”
- “What should I do if they change?”
- “How often should I check?”
Common Myths About Monitoring Chronic Diseases
Myth: I feel fine, so I don’t need monitoring.
Reality: Damage often happens silently.
Myth: More data is always better.
Reality: Too much data can hide real signals.
Myth: Any doctor can interpret my readings.
Reality: Context matters.
ChextrMD Fits Into Continuity-Based Clinical Monitoring
ChextrMD is built around one core belief: better outcomes come from long-term doctor–patient relationships, not one-off interactions. It is designed to support continuity of care between a patient and their own known physician.
This makes it especially relevant for patients with hypertension, diabetes, asthma, and multiple long-term conditions. These conditions do not need constant diagnosis. They need consistent supervision. ChextrMD focuses on:
- continuous access between physicians and their existing patients
- ongoing clinical guidance between visits
- monitoring oversight and follow-up
- safe, documented communication tied to an established care relationship
ChextrMD Aligns With Continuity-Based Monitoring
Clinical monitoring only improves outcomes when:
- someone is responsible for reviewing the data
- that person knows the patient’s history
- action is taken early and appropriately
ChextrMD supports this by helping doctors:
- stay connected to their patients between visits
- review monitoring data in context
- provide timely guidance without fragmenting care
The platform strengthens what already exists—the doctor–patient relationship.
ChextrMD is Designed for Premium, Relationship-Driven Care
ChextrMD is positioned for:
- busy professionals
- high-trust patients
- physicians who value long-term partnerships
These patients often:
- travel frequently
- manage demanding schedules
- limited time for repeated clinic visits
- value discretion, safety, and reliability
For them, continuity is not a luxury. It is a requirement.
ChextrMD Supports, Not Replaces, Clinical Visits
- extends care between appointments
- monitor stability between reviews
- supports follow-up after visits or hospital discharge
This positioning keeps care safe, ethical, and compliant with regulatory standards. It does not:
- diagnose new conditions
- replace physical examinations
- bypass established care pathways
ChextrMD Matters for Hypertension, Diabetes, and Asthma
These conditions require:
- longitudinal trend review
- medication safety over time
- early detection of drift
ChextrMD reduces silent deterioration and avoidable crises. It fits here by enabling:
- ongoing oversight by the same physician
- timely response to monitoring changes
- reduced gaps in follow-up
At its core, ChextrMD stands for:
Premium continuity of care—supporting doctors and their known patients with ongoing guidance, monitoring oversight, and trusted follow-up between visits.
Not fast care.
Not fragmented care.
But care that stays connected.
FAQs: Monitoring Hypertension, Diabetes, and Asthma
Q1: How often should blood pressure be checked at home?
There is no single schedule that fits everyone. For many patients, doctors recommend short monitoring periods rather than daily checks forever. A common approach is:
- measure blood pressure twice a day for 5–7 days
- repeat this once a month, or when treatment changes
- share the results with the same doctor or care team
This method shows true patterns without causing stress or fatigue. Daily long-term checking can increase anxiety and may lead to reacting to normal ups and downs. A doctor who knows your history can decide how often monitoring is really needed.
Q2: Is HbA1c enough for diabetes monitoring?
No. HbA1c alone is not enough. HbA1c shows average blood sugar over about three months, but it does not show:
- daily highs and lows
- episodes of low blood sugar
- how meals, stress, or illness affect you
Continuity matters because the same doctor can compare trends over time and adjust care safely, without over-treating or missing warning signs. Good diabetes monitoring usually combines:
- HbA1c tests
- home glucose readings (as advised)
- symptom review
- medication tolerance checks
Q3: Do asthma patients need monitoring if symptoms are rare?
Yes. Even when symptoms are rare, monitoring is important. Asthma can worsen quietly. Airways may become more sensitive before symptoms are obvious. Monitoring helps:
- detect early loss of control
- adjust preventer treatment in time
- reduce the risk of sudden severe attacks
A clinician who follows you over time can recognize patterns and seasonal triggers that others may miss. Monitoring may include:
- tracking symptom frequency
- noting night-time symptoms
- watching rescue inhaler use
Q4: Can one doctor safely manage all three conditions?
Yes. In many cases, one doctor or a small care team can safely manage all three. Continuity helps because:
- medications are reviewed together
- drug interactions are considered
- one condition is not treated at the expense of another
A doctor who knows the full picture can balance care carefully, with support from nurses or coordinators when needed. For example:
- some asthma treatments can affect blood sugar
- some blood pressure medicines may influence glucose levels
Q5: Why is continuity important when reviewing home monitoring results?
Numbers without context can be misleading. Seeing trends over time is safer than reacting to single readings. This reduces unnecessary medication changes and missed warning signs. Continuity allows the clinician to:
- know your normal range
- understand past responses to treatment
- tell temporary changes from real problems
Q6: What should patients do if home readings suddenly change?
Clear instructions on when and how to report changes should always be part of a monitoring plan. Patients should:
- note the readings and any symptoms
- avoid panic or self-adjusting medication
- contact their usual doctor or care team for guidance
A known clinician can decide whether the change is urgent or temporary.
Q7: Can monitoring become harmful if overdone?
Yes, if not guided properly. The goal is useful monitoring, not constant checking. A doctor who knows you can help find the right balance. Over-monitoring can:
- increase anxiety
- lead to overreaction
- cause confusion about what matters
Q8: Is home monitoring accurate?
Home monitoring can be accurate when:
- devices are validated
- patients are shown proper technique
- readings are reviewed regularly
Poor technique or faulty devices can give misleading results. This is another reason continuity and guidance matter.
Q9: What role do nurses or care coordinators play in monitoring?
Nurses or care coordinators play a vital role. This team-based approach keeps care responsive while maintaining continuity. They can:
- review readings first
- check adherence
- identify early concerns
- escalate to the doctor when needed
Q10: What is the safest takeaway for patients with these conditions?
Stay connected to a care team that knows you. Continuity turns numbers into protection. Monitoring works best when:
- plans are clear
- follow-up is consistent
- tesponsibility is shared, but ownership is clear
Monitoring Works Best When Care is Continuous
Hypertension, diabetes, and asthma do not shout when they worsen.
They whisper.
Clinical monitoring helps clinicians hear those whispers.
Continuity helps them understand what they mean. When the same care team follows a patient over time, numbers turn into insight, and insight turns into prevention.
For safer outcomes, fewer emergencies, and better long-term health, monitoring must always stay connected to continuous, trusted care. 🫶🫂
For further insights, revisit our main guide on: Clinical Monitoring and Better Outcomes Through Continuity: How Continuous, Person-Centered Care Cuts Risk, Costs, and Readmissions

